Have you become more interested in health research over the last year? If so, you’re not alone.

With the COVID-19 pandemic putting a spotlight on the nation’s wellbeing, more of us than ever are realising the importance of medical research – and coming to understand the vital role it plays in shaping our society and healthcare systems.
Why is health research so important?
Health research is critical to making sure that we’re providing the best possible care for everyone – both today, and in the future.
Whether our knowledge is gained through clinical trials, equipment testing, surveys, questionnaires or data analysis, the answers we find help us improve our processes, healthcare and make positive change.
In fact, some of the most important medical discoveries over the past 80 years – including aspirin, penicillin and the contraceptive pill – would never have come about if it weren’t for the hard work of scientists, researchers and volunteers.
As the nation’s largest funder of health and care research, the NIHR is dedicated to gathering the robust knowledge which makes such discoveries possible.
It’s thanks to health research that we’re able to:
- Improve diagnosis time and accuracy
- Better understand how to prevent conditions from developing
- Fight new strains of viruses
- Provide life-saving treatments and procedures
- Ease suffering and improve care
Five amazing health research breakthroughs
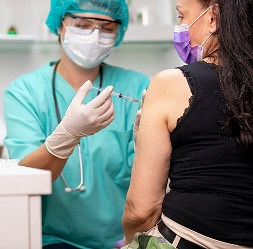
1. The Oxford/AstraZeneca COVID-19 Vaccine
It was the discovery the world had been waiting for: in 2020, the Oxford/AstraZeneca vaccine was found to be effective at preventing COVID-19 and offering a high level of protection.
Key facts
- The vaccine was developed by biopharmaceutical company AstraZeneca alongside the University of Oxford. Development of the vaccine was funded by the UK Research and Innovation (UKRI) and the Department of Health and Social Care through the NIHR.
- Clinical trials enrolled more than 24,000 participants from around the world – from the UK to South Africa.
- The vaccine was made from a weakened version of a common cold virus (adenovirus), genetically modified to be unable to grow in humans.
- Trials showed that the vaccine was 70.4% effective – or 90% effective when administered in a half dose followed by a full dose – and that it could also prevent transmission.
- Within just 5 months of being approved, around 17 million people in the UK and EU had received a dose of this life-saving vaccine.
2. The human liver repaired using lab-grown cells
In 2021, in the first procedure of its kind, researchers demonstrated a new technique to show that a damaged human liver could be repaired with mini bile-ducts grown in a lab.
Key facts
- With a shortage of liver donors, researchers supported by the NIHR Cambridge Biomedical Research Centre aimed to develop an alternative to transplantations.
- Malfunctioning bile ducts, which act as the organ’s waste disposal system, are the cause of 70% of liver transplants in children, and a third in adults.
- The researchers used this technique to grow new ‘mini-bile ducts’ in the lab.
- Research showed that biliary cells from the human gallbladder could be converted into bile duct cells to replace and repair the damaged bile ducts.
- This is the first time a procedure of this kind has been used on human organs and this breakthrough could increase the number of suitable donor livers.
- This approach could also be applied to range of organs and diseases, to further accelerate cell-based therapy research.
3. The super effective single-dose breast cancer treatment
Led by researchers at University College London in 2020, a pioneering breast cancer therapy was found to be as effective as conventional treatment – while taking just 30 minutes.
Key facts
- The study was funded by the NIHR’s Health Technology Assessment Programme and Cancer Research UK, and involved 32 hospitals in ten countries.
Results confirmed the effectiveness of Target Intraoperative Radiotherapy (TARGIT-IORT), a treatment which is delivered directly after tumour removal and which acts as both surgery and radiation treatment at once. - TARGIT-IORT works via a small ball containing a single dose placed inside the breast.
- The conventional treatment for breast cancer – external beam radiotherapy (EBRT) – takes 3-6 weeks of daily treatment; TARGIT-IORT takes just 20-30 minutes.
- TARGIT-IORT also has fewer radiation-related side effects, a better cosmetic outcome and leads to a substantial reduction in deaths from causes other than breast cancer.
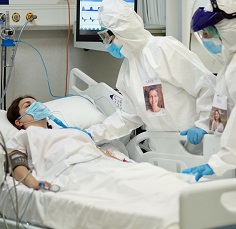
4. The steroids and arthritis drugs saving the lives of COVID-19 patients
Researchers on the NIHR-funded and supported RECOVERY study (Randomised Evaluation of COVID-19 therapy) which examined multiple drugs and their effects on COVID-19 recovery for hospitalised patients, discovered that the steroid dexamethasone and the arthritis treatment tocilizumab were able to dramatically reduce the risk of death for patients with severe COVID-19.
Key facts
- In 2020, the dexamethasone study compared the results of 2104 patients randomly selected to receive dexamethasone once per day for ten days, and 4321 patients randomly selected to receive usual care alone
- Dexamethasone was found to reduce the risk of 28-day mortality by 17%, with a significant trend showing greatest benefit among those on ventilators
- Dexamethasone has since been reported to have saved 22,000 lives in the UK and an estimated one million worldwide in the treatment of COVID-19
- In 2021, tocilizumab was found to reduce the length of hospital admission and the risk of patients requiring mechanical ventilation
- 2022 patients were randomly allocated to receive tocilizumab by intravenous injection. Results were compared with 2094 patients randomly allocated to usual care alone.
- The study showed that for every 25 patients treated with tocilizumab, one additional life would be saved.
5. The oral antibiotic advancing cystic fibrosis treatment
The conclusion of a 10-year trial in 2020 revealed that oral antibiotics could successfully be used to treat a common cystic fibrosis complication at home.
Key facts
The study was funded by NIHR, sponsored by University Hospitals Bristol and Weston NHS Foundation Trust, and developed with researchers from The University of Nottingham’s School of Medicine.
- 286 patients took part in the study, which was conducted over 70 cystic fibrosis centres across the UK and Italy.
- Patients with cystic fibrosis are prone to infection by a bacterium called Pseudomonas aeruginosa, which causes chronic destructive lung infections.
- The study found that traditional oral antibiotics are just as effective as intravenous antibiotics in tackling Pseudomonas aeruginosa.
- No longer requiring intravenous medication means that patients can be treated in the comfort of their own home, improving the quality of life for many people with cystic fibrosis.
Getting involved with health research
From the life-saving procedures to the discoveries that have improved treatment, none of these breakthroughs in health research would have been possible without the support of volunteers.
That’s why it’s so important to get as many people as possible interested in research – because only through working together will we keep advancing the field of medical care.
There are many different types of health research and ways to get involved, and you don’t need to have a medical condition in order to help with research.
Ready to see how you can make a difference in health research? Find a study in your area today.
Related articles
- Different ways to take part
- Explore NIHR alerts which are plain English summaries of the latest research findings
- Why take part in research?